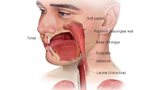
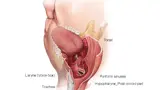
Radiation Therapy for Hypopharyngeal Cancer
The most common radiation therapy approach for Hypopharyngeal Cancer is called external beam radiation. This type of radiation therapy applies radiation from outside the body.
Radiation therapy can be used in the following ways:
Definitive
This is a curative treatment option for people with Hypopharyngeal Cancer. The aim of this treatment is to preserve the larynx and its function. It is an alternative to surgery, which may involve removal of the voice box (laryngectomy). Radiation therapy comprehensively treats the cancer of the hypopharynx, the surrounding region and the lymph nodes at both sides of the neck. Radiation therapy is delivered daily (no treatment on weekends) for 7 weeks and can be given as:
- definitive radiation therapy alone; or
- definitive radiation therapy with concurrent chemotherapy (adding chemotherapy to radiation therapy (chemoradiation) to make it more effective).
Adjuvant
This is when radiation therapy is given after the surgical removal of the Hypopharyngeal Cancer. Adjuvant Radiation Therapy is used as an additional treatment to kill cancer cells that may not have been removed during surgery and may still be present in the hypopharynx and in the lymph nodes at both sides of the neck. It usually starts about 4 weeks after surgery to allow recovery from surgery. Radiation therapy treatment usually lasts for about 6 weeks. Sometimes chemotherapy is added to the adjuvant radiation therapy (chemoradiation) to make it more effective.
Palliative
Radiation therapy is also used to relieve symptoms of advanced Hypopharyngeal Cancer. Symptoms that may require palliative radiation therapy include pain, bleeding, breathing and swallowing difficulties.
How do I Prepare for Radiation Therapy?
You will meet with many members of the cancer care team, who will help you learn how to look after yourself through radiation therapy, recovery and long term follow-up. They will also talk to you about side effects and how to manage them. It may be helpful to write down questions as they come up, so you can ask anyone in your cancer care team when you see them.
Therapy Mask-Making and Simulation
- Radiation therapy is a precise treatment. In order to make sure, that the cancer is covered by the treatment, you will need to be very still during the treatment, usually for about five minutes. A radiation therapy mask that is made to fit perfectly to your shape, will be put on you during each treatment to help the machine target where the cancer is.
- You will have a planning CT scan (and sometimes other scans) with the mask on. Your radiation oncologist and radiation therapists will use these scans with all your other clinical information to develop a radiation therapy plan just for you (a personalised plan). Your plan will be checked by the radiation therapy and radiation oncology physics team before it is ready to be used for your treatment. This whole process can take approximately 2-3 weeks.
Teeth and Mouth Care
Dental extraction may be needed to remove any broken or infected teeth before radiation therapy. It is important to take out any broken or infected teeth before radiation therapy. Taking out unhealthy teeth after radiation therapy can cause problems with the jaw bone.
Diet, Nutrition and the role of your Dietitian
Your cancer and its treatment can make it hard to eat and drink. Your doctor will recommend you see a dietitian to maximise your nutrition during treatment as well as while you are recovering. Sometime feeding tubes may be recommended depending on the area being treated and the dose of radiation therapy.
There are two common types of feeding tubes:
- Gastrostomy tube (sometimes called a PEG tube): this type of tube is inserted through your abdominal wall into your stomach, with part of the tube staying outside the stomach. A syringe can be attached to the tube to give you food this way if needed. The tube is inserted using a camera through the mouth into the stomach (gastroscopy) or using a CT scanner to guide insertion directly through the skin. If a PEG tube is needed, your doctor will organise this before starting your radiation therapy.
- Nasogastric tube: this type of tube goes through the nose down into the stomach and is usually used for short periods (days or weeks). A nasogastric tube can be inserted at any time (before, during or after treatment).
Speech, Voice and Swallowing
Your cancer and its treatment can make swallowing and speech difficult. Your doctor will recommend you see a speech pathologist, who can help you with ways to manage swallowing and communication difficulties, during and after treatment. Your speech pathologist will also help with your voice rehabilitation during and after treatment.
There are many other aspects of supportive care that are available, ask your doctor if you have any specific needs.
Side Effects of Radiation
The side effects of radiation therapy start around two weeks into treatment and progress through treatment to peak in the last week or just after treatment ends. The side effects start to improve 2-3 weeks after the end of treatment.
Side effects associated with radiation therapy depend on:
- the dose of radiation therapy
- the area being treated
- whether or not chemotherapy is added to the radiation.
Each person responds to radiation therapy differently. Some people may experience a few side effects while others may not experience any at all. The following are some common side effects of radiation therapy.
- tiredness
- hoarse voice
- skin irritation in the treated area e.g. redness, dryness and itching, weeping skin, scaling or sometimes skin breakdown (sores)
- pain on swallowing or difficulty with swallowing
- irritation in the throat progressing to sore throat requiring pain killers
- dry moth and throat (with advanced stage hypopharyngeal cancer treatment).
Most side effects are short lived and may go away within 4–6 weeks of finishing radiation therapy. Some side effects may last for months after you finish radiation therapy and some may be permanent.
Uncommon side effects of radiation therapy for hypopharyngeal cancer include aspiration (coughing and infection due to food/fluids trickling into your windpipe) and swelling in the airway causing obstruction and difficulty breathing.
Once your radiation therapy ends, you will continue to have follow-up appointments so that your doctor can check your recovery and monitor any side effects that you may have. Your doctor will arrange for a PET scan about 12 weeks after finishing radiation therapy to make sure the cancer has completely gone.
Your doctor may recommend that you receive specific supportive care to help during your treatment and recovery.
Chemotherapy for Hypopharyngeal Cancer
Chemotherapy works by destroying or damaging cancer cells. For Hypopharyngeal Cancer, it is usually given into a vein through a needle with a cannula (tube) attached.
There are a number of ways that chemotherapy may be used to treat Hypopharyngeal Cancer including:
Definitive
Sometimes chemotherapy is added to definitive radiation therapy (chemoradiation). It is usually used for advanced stage hypopharyngeal cancers. This may be given once every 3 weeks or once a week throughout the duration of radiation therapy. The addition of chemotherapy makes the radiation more effective at killing cancer cells but also leads to increased side effects in most patients.
Adjuvant
This is when chemotherapy is given after surgery, in combination with radiation therapy (chemoradiation). This may be given once every 3 weeks or once a week or every day that radiation therapy is given. The addition of chemotherapy makes the radiation more effective at killing cancer cells but also leads to increased side effects in most patients.
Neo-Adjuvant
This is when chemotherapy is given before surgery or radiation therapy to help shrink large cancers and make them easier to remove during surgery or target with radiation therapy.
Palliative
This is used when the cancer is incurable. The cancer may be too large or has spread too much to be removed by surgery. Palliative chemotherapy helps to slow the growth of cancer and reduce symptoms. It is important to remember that palliative chemotherapy is not as intense as other types and is much less likely to have significant side effects.
Before you start treatment, your medical oncologist will choose one or more chemotherapy medications that will be best to treat the type of cancer you have.
The chemotherapy medications your doctor chooses may depend on:
- whether the treatment is curative or palliative
- when it is used
- your medical history
Side Effects of Chemotherapy
The side effects of chemotherapy depend on the medication used and and how much you are given by your doctor (the dose). The most common medications used are called cisplatin, carboplatin and cetuximab.
Each person responds to chemotherapy differently. Some people may experience a few side effects while others may not experience any at all. The following are common side effects of chemotherapy:
- a feeling of wanting to vomit (nausea) or vomiting
- more side effects of radiation, if you have chemotherapy at the same time as radiation
- most of these side effects are short lived and may go away once you finish chemotherapy. Some side effects can take months or years to improve or may be permanent
Once your radiation therapy ends, you will have regular follow-up appointments so that your doctor can check your recovery, make sure the cancer has not returned and monitor and treat any side effects that you may have.
Your doctor may recommend that you receive some specific supportive care to help during your recovery.
- loss of feeling in the fingers and toes
- kidney damage (caused by some medications)
- hearing loss/thinning
- ringing in the ears
- rash
- higher risk of infection (if the chemotherapy reduces the number of white cells in the blood)